About
Welcome to the Syed Lab

As a pediatric gastroenterologist working as part of a group of dynamic colleagues, I take care of children who present to our clinic with a wide array of digestive disorders. These children are often not growing well, have diarrhea, abdominal pain, or a myriad of other symptoms. As part of their clinical care, we often need to do diagnostic investigations to better evaluate their gut structure and function as part of their evaluation. While we know every child is unique and has their own disease experience, we are currently limited in how much we can individualize our diagnostic and subsequent management of each patient. Since treatment is not individually tailored based upon risk, significant variability in patient responsiveness to treatment and disease progression exists. Understanding these distinctions matters because individualized insight into specific disease associations would facilitate risk-stratification and more efficient care with the potential earlier diagnoses and personalized management – we call this “precision medicine.”
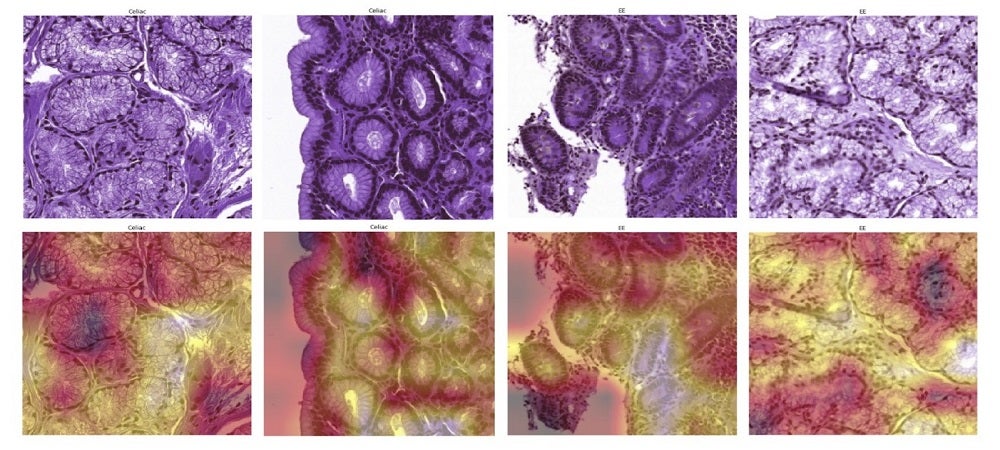
In my role as a pediatric global health investigator, I am constantly stunned by the gaps between who benefits from key advancements in medicine and who does not. In 2021, why are children living in the poorest parts of the world suffering from Environmental Enteropathy? An entirely preventable condition, EE, a non-specific inflammatory condition of the small intestine, is now considered to be the primary driver for linear growth failure or stunting. EE afflicts approximately 160 million children under five years of age worldwide. Stunting serves as a clinical marker for lifelong impairments in physical growth, neurocognitive development, vaccine immunological response, and socioeconomic potential. EE is attributed to chronic exposure to enteropathogens, with subsequent mucosal inflammation, villous blunting, damaged barrier function, and reduced nutrient absorption. Unbelievably, to date, no diagnostic biomarker(s) or definitive treatments exist for EE.
How can we solve these problems?
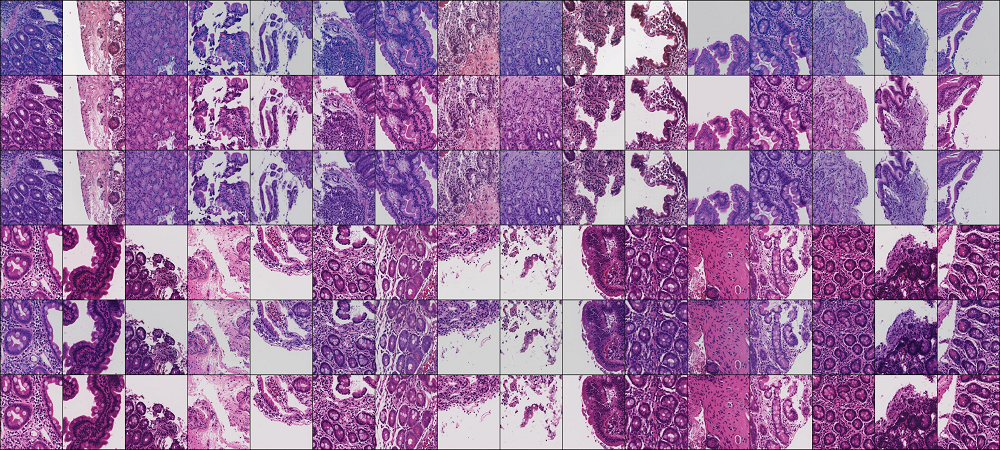
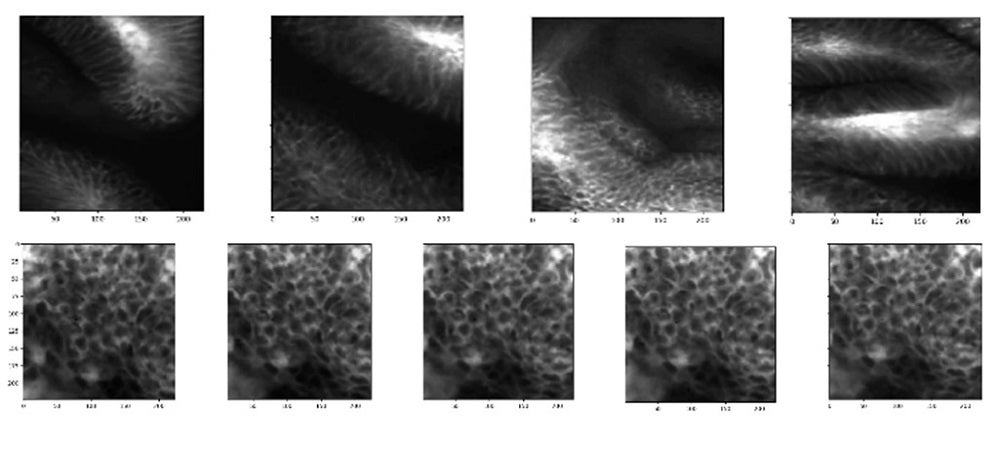
Our lab hopes to contribute to addressing these challenges by our studies of intestinal structure and function with a specific focus on enteropathies. We leverage machine learning (ML) image analyses/computer vision analytics for better feature discovery in GI diagnostic modalities such as digital pathology, endoscopy, and radiology to study intestinal structure. We have also been using molecular ‘omic tools to help understand the black box of ML-driven predictive models, which is a critical priority given the translational patient-centered nature of our work. Our study of intestinal function has involved working with collaborators to use computational metabolic modeling to develop druggable targets and disease biomarkers.
The Syed Lab’s overarching goal is to empower clinicians and patients to make shared, precision medicine based on therapeutic decisions using individual patient data. Twenty years from now, we want to look back and consider how behind we were. Our current and future efforts are driven by how do we give back? How do we have an impact beyond our immediate selves? How can we improve the lives of the vulnerable children entrusted to our care?