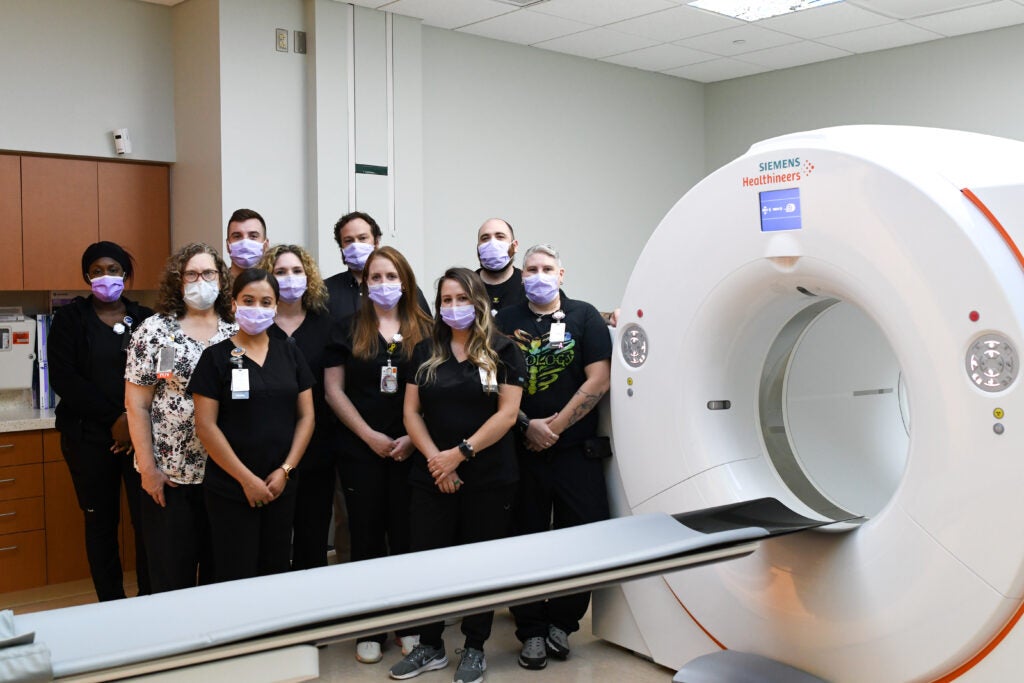
The patient care team in the UVA Division of Nuclear Medicine and Molecular Imaging is small—just twelve people—but they play an outsize role in the lives of their patients.
These technologists, nurses, access associates and coordinators who work to schedule, image and treat patients come to develop deep relationships with the people they serve. And they get to see the extraordinary impact that the care they provide has on their patients’ lives.
Adam Campbell, Nuclear Medicine Technologist, has been at UVA for just a year and a half, but he has already been affected by the close relationships he has developed with patients. “We see people at some of their darkest times,” Campbell says, “And we are able to be a light for them, either around their diagnosis or during a recovery time.”
For the Nuclear Medicine team, getting to know the people they care for and being a light in dark times is what makes their work so fulfilling.
Nuclear Medicine 101
Hunter Beverley is the Supervisor of Nuclear Medicine and PET/CT. He leads a team of six technologists as well as a lead QA/QT technologist. They work closely with Jeri Pugh, RN, the Nuclear Medicine Nurse Coordinator, administrative coordinator Tamika Hassel, and two front desk associates, Jeff Fry and Lori Diaz.
“A lot of people ask how we’re different from CT,” Beverley says. “I tell them that CT is anatomical but nuclear medicine is physiological.”
Nuclear medicine imaging shows how organs or other systems in the body are functioning in real-time. Patients are injected with specific types of molecules called radiotracers, which are absorbed by the parts of the body that need to be examined. They give off a small amount of radiation which a nuclear medicine camera can read. This real-time, functional view gives doctors a better understanding of tumors, infections, organ function and blood circulation.
But the most exciting developments in nuclear medicine, as Beverley sees it, lie in new forms of treatment. “As nuclear medicine is going into the future, not only are we able to image and help diagnose patients, but we are now involved in treatment,” he says. This rapidly growing field of therapy is called theranostics, and it’s among the most exciting and cutting-edge areas in medicine.
At UVA, the nuclear medicine division performs new targeted treatments for neuroendocrine tumors and prostate cancer, with many more treatments on the horizon.
By the Numbers
Currently, UVA has four nuclear medicine cameras, one PET/CT scanner and two treatment rooms. On a normal day, the division will image about 18 patients with PET/CT and another 15 to 20 patients with the other cameras.
That may not sound like a lot of patients, but it’s important to note that nuclear medicine scans take a long time.
“The average nuclear medicine scan time is 20 minutes,” Beverley says. “But PET scans take two hours, with an IV, injection of the radiotracer, and then scanning. Bone scans are a three-hour process. Some exams take three days, with an injection on day one, and then two days of imaging.”
With exams this complex and time-consuming, technologists and other team members must work closely together to care for their patients.
A Patient’s Journey Through Nuclear Medicine
The front desk team is the public face of Nuclear Medicine. They check patients in and alert clinical staff that they have arrived. Technologists bring patients back to a prep room, prepare them for their exams, bring them to the scanners and perform the imaging exams using the complex machinery. If injections or IVs are needed, either a technologist or a nurse will take care of it.
After imaging, technologists will check on the patients and monitor them for any adverse effects up until the time they are ready to leave. This means that technologists are with patients the entire time they are here.
“We keep techs with the same patients each time they come in,” says Beverley. “We don’t want patients to have a new team each visit. We want them to know us and know that the same person will be taking care of them each time they are here.”
Much of the work with patients between visits—scheduling appointments and labs, entering orders, and doing patient education—is done by Jeri Pugh, the Nuclear Medicine Nurse Coordinator. Beverley calls this work “the big-picture items” that make it possible for patients to be ready to be imaged or treated safely when they arrive in the division.
Am I Going to Glow?
As the first point of contact for most patients referred to nuclear medicine, Pugh hears their initial concerns and fears, especially around radiation and its effects. A question she has heard many times once patients learn about radiation, is “am I going to glow?” She reassures them that the exams and treatments her team performs are safe.
Pugh came to the division in April 2021, after eleven years in the ER and a long-term care facility. Just like her patients, Pugh didn’t know much about Nuclear Medicine when she started. But she quickly learned a huge amount of information, aided by her physician and technologist colleagues.
“I am still continuing to learn, which is something I love about this job,” she says. “Its a growing field with a lot of new treatments and imaging techniques coming out.”
“The most rewarding part of my job is getting to know patients over time,” she continues, “as often patients come back for repeat imaging and restaging. It’s not just a one-time visit—we get to see patients through highs and lows, developing relationships with them over the years.”
Her patients come from a wide geographic area and different socioeconomic groups, which brings challenges. In particular, coordinating precautions after receiving radioactive treatment can be difficult for some patients, like those with small children who don’t have other childcare options, for example, or who share a room with several people and can’t stay the recommended distance away from them. In those cases, Pugh helps to organize and coordinate alternative places for them to stay for a few days, or make child care arrangements.
“We come together to do everything we can for a patient,” she says. “We work well together to take care of a patient as a whole. The friendly attitude here really makes it such a positive work environment to be in. And I think patients can feel that. When you go in somewhere and staff are unhappy, you can tell. Our satisfaction goes a long way towards our patients’ satisfaction.”
Going the Extra Mile
Beverley agrees with Pugh. “Our team does really well with taking care of our patients and making sure they have what they need,” he says. “We have protocols for everything. But sometimes things fall outside of those protocols, so you also have to know how to use the resources you have. How will you work with other departments to take care of a patient? What other people in the health system can you call upon?”
“Say a patient’s car breaks down the day before an exam,” he continues. “We will call social workers to make sure they can get a ride here. We always ask ‘How can we help? How can we go one step further to help?’”
Going the extra mile is something that patients notice.
“That’s the biggest feedback I hear from patients,” Beverley says. “They say ‘Where is ____? They took such good care of me.’ Or I’ll get a patient note that might say: ‘So-and-so did an outstanding job today. He was able to relate to my son and talk with him about skateboarding.’ It’s more than just ‘he did a great job.’ It shows me that we made a real impact on that patient.”
Technologist Adam Campbell agrees that the bond he forms with patients makes a real different for their care. “Until working here, I never knew how deep of a bond you can form with a patient from just working with them for a few hours,” he says. “But now I see how much that time together can mean.”

Comments