Cardiothoracic Division
About

Dr. Karen Singh speaking with Dr. Jessica Zvara outside of the OR.
The Cardiothoracic Anesthesiology Division at the University of Virginia (UVA) provides anesthesia and perioperative care for adult patients undergoing a variety of complex cardiac, thoracic and vascular surgical procedures. Our Division faculty is excited to optimize patient care to give our patients the best possible clinical experience.
Cardiac
Cardiac anesthesiologists routinely perform anesthesia for coronary artery bypass surgery, complex valvular heart disease, thoracic aortic surgery, ventricular assist device placement and heart transplantation. In addition, we care for patients undergoing transcatheter aortic valve replacement (TAVR) and other transcatheter valve procedures as part of the robust Heart Valve Program at UVA. Our Anesthesiology Perioperative Echocardiography Service performs and interprets all adult cardiac surgery transesophageal echocardiography (TEE) and point of care echocardiography in the operating room and in the recovery unit (see Clinical Programs).
Thoracic
Our thoracic anesthesiology team provides comprehensive perioperative care for a wide variety of thoracic procedures, including lung transplantation and surgery of the esophagus, stomach, lungs, mediastinum, and the thoracic spine. Thoracic procedures include open and minimally invasive procedures, including classical video assisted thoracoscopic surgery, as well as robotic surgeries.
Vascular
Our vascular anesthesiology team administers anesthesia for patients undergoing complex vascular surgery with a patient-centered approach. We have successfully developed and implemented cardiac and thoracic enhanced recovery after surgery (ERAS) programs. We enhance patient care through collaboration among the cardiothoracic and the vascular surgery teams, as well as with nursing staff who are essential to our progress. Teamwork allows us to give our patients the best possible outcomes.
A Message from the Cardiac Anesthesia Division Chief

John McNeil, MD, MBA, Cardiac Anesthesia Division Chief
We have a very talented group of Cardiothoracic Anesthesiologists here at UVA. Our members have wide-ranging interests and skills in education, research, and clinical care. Many members in our division have been the recipients of teaching awards. Research interests are varied and include coagulopathy, echocardiography, advanced monitoring, medical student and resident education, and thoracic anesthesia.
Most of our division members hold National Board of Echocardiography certification in Advanced Perioperative TEE. Our goal is to provide excellent resident education, and several in our division regularly teach cardiothoracic clinical skills in the simulation center and give formal lectures to prepare residents for their cardiac anesthesiology rotation. Many of us also teach transesophageal echocardiography and point-of-care ultrasound (POCUS) to residents through formal lectures as well as hands-on instruction in the simulation center and perioperative setting.
A Message from the Thoracic Section Chief

Randal Blank, MD, PhD, Thoracic Anesthesia Section Chief
Thoracic division faculty are exceptionally committed to high quality patient care, education of medical students and residents, and research efforts to improve and advance medical knowledge. Division faculty have extensive expertise in a diverse array of specialized care modalities, including thoracic epidural analgesia, bronchoscopy, advanced airway management techniques, fiberoptic guided placement of lung isolation devices, lung ultrasound, and transesophageal echocardiography.
We are a group of experienced perioperative physicians who are actively engaged in advancing the clinical practice of thoracic anesthesia, teaching the next generation of thoracic anesthesiologists and advancing knowledge through clinical and translational research. Division faculty are involved in education and teaching at the national level and are engaged in collaborative research projects with other leading investigators at home and abroad.
A Message from the Vascular Section Chief

Jessica Zvara, M.D.,
Vascular Anesthesia Section Chief
Dr. Jessica Zvara was named Vascular Anesthesia Section Chief in March 2024. The vascular anesthesia experience at UVA is excellent. The new Aortic Center at UVA brings in many patients with complex aortic disease. With vascular surgery volumes increasing, residents have the opportunity to care for high acuity patients undergoing a variety of vascular procedures, ranging from limb salvage, to dialysis access, to bypass surgeries, to multi-stage hybrid aortic repairs.
Residents are supervised by faculty from many divisions, with dedicated teaching of classic vascular anesthesia principles (preoperative evaluation, the physiology of cross-clamping, spinal drains, coagulation) during high-risk cases. There is an opportunity to hone point-of-care ultrasound (POCUS) technique and non-invasive continuous blood pressure monitoring familiarity during less demanding surgeries. Our division works closely with our vascular surgery colleagues and the rest of the perioperative team to provide the best care possible to all patients undergoing vascular procedures at UVA.
Our Division
-
John S. McNeil, MD
Cardiothoracic
-
Randal S. Blank, MD, PhD
Cardiothoracic
-
Jessica Zvara, MD
Cardiothoracic
-
Paul D. Gallo, MD
Critical Care, Cardiothoracic
-
Amanda M. Kleiman, MD
Cardiothoracic, Liver Transplant, Obstetrical
-
Michael Mazzeffi, MD, MPH, MSc, FASA
Critical Care, Cardiothoracic
-
Sachin H. Mehta, MD
Obstetrics,
Cardiothoracic
-
Robert M Ricketts III, MD
Pediatric, Cardiothoracic
-
Joshua Roach, MD
Critical Care, Cardiothoracic
-
Karen E. Singh, MD, FASE
Cardiothoracic
-
D. Keegan Stombaugh, MD
Critical Care, Cardiothoracic
-
Robert H. Thiele, MD
Critical Care, Cardiothoracic
-
Susan M. Walters, MD
Cardiothoracic
Cardiac Anesthesia
We provide anesthesia for approximately 700 cardiopulmonary bypass cases annually at UVA, including CABG, valve repair and replacement, LVADs, ascending aortic surgery, heart and lung transplantation. In addition, we cared for over 300 transcatheter valve patients in the last year. Our team often anesthetizes patients placed on ECMO who require procedures or surgery in the operating room.
We have a robust ERACS (enhanced recovery after cardiac surgery) program, and long-standing practices such as perioperative glucose optimization and targeted transfusion with point-of-care coagulation studies. These have helped us provide excellent patient care over the years. We consistently look for ways to improve patient care and are currently working with a multidisciplinary team in order to optimize blood conservation in cardiac surgery at UVA.
Anesthesiology Perioperative Echocardiography Service
The Anesthesiology Perioperative Echocardiography Service performs and formally interprets transesophageal echo (TEE) for all adult cardiac surgery cases at UVA. The service also provides point of care transthoracic and transesophageal exams for hemodynamically unstable patients in the operating room and in the post-anesthesia recovery unit. All covering faculty are certified by the National Board of Echocardiography in Advanced Perioperative TEE. This service is an excellent format for formal TEE and POCUS teaching for residents on their TEE rotation.
Thoracic Anesthesia
Members of the thoracic anesthesia team provide care for patients planning and undergoing complex and high risk procedures including lung transplantation, esophagectomy, complex resections of the lung and major conducting airways, tracheobronchial resection and reconstruction, high risk mediastinal mass resection and chest trauma. Our team collaborates closely with thoracic surgeons and other interventionalists to plan complex cases and optimize the perioperative patient experience. We are committed to the highest level of care throughout the perioperative process and have pioneered an enhanced recovery program (ERP) for thoracic surgery which has reduced hospital stay and costs while dramatically reducing opioid utilization in both the short and long term. We review the ERP quarterly in an ongoing effort to optimize the program, incorporating advances in the field. This ERP has served as the model for similar programs at other leading institutions.
Vascular Anesthesia
Our division cares for patients undergoing many types of major vascular surgery. Last year UVA performed approximately 230 major open and endovascular aortic cases. Complex endovascular procedures are increasing in number. Currently, our division is working with a multidisciplinary team to create an ERAS pathway for open abdominal aortic surgery cases.
Current Clinical Research Projects
International Multicenter ANH Randomized Control Trial
Mike Mazzeffi, MD; Karen Singh, MD; and John McNeil, MD
UVA is participating in a multicenter randomized control trial comprising 2000 cardiac surgery patients worldwide. Globally, around 900 participants have been enrolled, with UVA contributing 29 participants to date. The study aims to shed light on Acute Normovolemic Hemodilution (ANH) and its impacts on factors such as transfusion requirements, bleeding, and acute kidney injury (AKI). ANH involves the removal of 1-2 units of a patient’s blood before heparinization, replacement with crystalloid as needed, and the subsequent return of the patient’s blood after cardiopulmonary bypass/heparin reversal. This technique is used to minimize blood loss and the need for blood transfusion.
Near Infrared Spectroscopy
Robert Thiele, MD
We study the use of near infrared spectroscopy (NIRS) to measure the oxidation state of cytochrome aa3, the terminal component of the electron transport chain. Our ultimate goal is to detect brain ischemia at the level of the tissue itself, rather than relying on hemoglobin oxygenation which is really only a surrogate marker. Our initial work utilized “broadband NIRS” but we have shifted towards more sophisticated time-domain and frequency-domain techniques that rely on laser light sources. This work is led by Dr. Robert Thiele, was originally funded by the Society of Cardiovascular Anesthesiologists and is now funded by the NIH (National Institute of Biomedical Imaging and Bioengineering).
Thoracic Research
Randal S. Blank, M.D., Ph.D.
We are currently engaged in a number of research efforts in various subfields of thoracic anesthesia and respiratory medicine. These include the impact of one lung ventilation management on postoperative outcomes, management of mediastinal mass syndrome, the role of driving pressure in the development of postoperative pulmonary complications, the effects of alveolar hyperoxia and systemic hyperoxemia on postoperative complications, mechanical power delivery to the respiratory system, and geospatial factors and pulmonary complications after lung resection surgery.
Recent Publications
McNeil JS, Singh KE, Gallo PD, Gehle B, Saunders MB, Mazzeffi MA. Medical Malpractice Claims Related to Performance of Transesophageal Echocardiography by Anesthesiologists. J Cardiothorac Vasc Anesth. 2024 Jan;38(1):118-122. PMID: 37923595. Epub 2023 Oct 06
Stombaugh DK, Singh K, Malek A, Kleiman A, Walters S, Zaaqoq A, Dawson M, McNeil JS, Kern J, Mazzeffi M. Preoperative Alcohol Use, Postoperative Pain, and Opioid Use After Coronary Artery Bypass Surgery. J Cardiothorac Vasc Anesth. 2024 Apr;38(4):957-963. PMID: 38310067. Epub 2024 Jan 22
Singh K, Tsang S, Zvara J, Roach J, Walters S, McNeil J, Jossart S, Abdel-Malek A, Yount K, Mazzeffi M. Intraoperative Methadone Use Is Associated With Reduced Postoperative Pain and More Rapid Opioid Weaning After Coronary Artery Bypass Grafting. J Cardiothorac Vasc Anesth. 2024 Aug;38(8):1699-1706. PMID: 38876810. Epub 2024 May 15
Kim J, Yoon S, Song IK, Lee K, Hwang W, Kim H, Lee DK, Lim HK, Kim SH, Lee JW, Hong B, Blank RS, Pedoto A, Popescu W, Theresa G, Martin AK, Patteril M, Pathanasethpong A, Thongsuk Y, Pisitpitayasaree T, Huang A, Yu H, Kapoor PM, Kim K, Chi SA, Ahn HJ. Recurrence-free survival after curative resection of non-small cell lung cancer between inhalational gas anesthesia and propofol-based total intravenous anesthesia: a multicenter, randomized, clinical trial (GAS TIVA trial): protocol description. Perioper Med (Lond). 2024 Jul 23;13(1):79. PMID: 39039548. Epub 2024 Jul 23
Fox WE, Kleiman AM, McNeil JS, Blank RS. Entangled iliac vein stents in the tricuspid valve. Can J Anaesth. 2023 Oct;70(10):1701-1702. PMID: 37434069. Epub 2023 Jul 11
Ranjha SA, Pressler MP, Blank RS, Schirmer BD, Lesh RE. Acute Respiratory Failure Complicating Endoscopic Sleeve Gastroplasty: A Case Report. A A Pract. 2023 Oct 1;17(10):e01724. PMID: 37801666. Epub 2023 Oct 06
Young AM, Viktorsson SA, Strobel RJ, Rotar EP, Cramer C, Scott C, Carrott P, Blank RS, Martin LW. Five-Year Sustained Impact of a Thoracic Enhanced Recovery After Surgery Program. Ann Thorac Surg. 2024 Feb;117(2):422-430. PMID: 37923241. Epub 2023 Nov 03
Yoon S, Nam JS, Blank RS, Ahn HJ, Park M, Kim H, Kim HJ, Choi H, Kang HU, Lee DK, Ahn J. Association of Mechanical Energy and Power with Postoperative Pulmonary Complications in Lung Resection Surgery: A Post Hoc Analysis of Randomized Clinical Trial Data. Anesthesiology. 2024 May 1;140(5):920-934. PMID: 38109657
Kim J, Yoon S, Song IK, Lee K, Hwang W, Kim H, Lee DK, Lim HK, Kim SH, Lee JW, Hong B, Blank RS, Pedoto A, Popescu W, Theresa G, Martin AK, Patteril M, Pathanasethpong A, Thongsuk Y, Pisitpitayasaree T, Huang A, Yu H, Kapoor PM, Kim K, Chi SA, Ahn HJ. Recurrence-free survival after curative resection of non-small cell lung cancer between inhalational gas anesthesia and propofol-based total intravenous anesthesia: a multicenter, randomized, clinical trial (GAS TIVA trial): protocol description. Perioper Med (Lond). 2024 Jul 23;13(1):79. PMID: 39039548. Epub 2024 Jul 23
Young AM, Strobel RJ, Rotar EP, Kleiman A, McNeil JS, Teman NR, Hawkins RB, Raphael J, Mehaffey JH. Perioperative acetaminophen is associated with reduced acute kidney injury after cardiac surgery. J Thorac Cardiovasc Surg. 2024 Apr;167(4):1372-1380. PMID: 36207161. Epub 2022 Sep 13
Ramarapu S, McNeil J, Tanaka KA, Vandyck K. Diagnosis of Microvascular Bleeding After Cardiopulmonary Bypass-A Game of Hide and Seek. J Cardiothorac Vasc Anesth. 2023 Aug;37(8):1510-1511. PMID: 37100638. Epub 2023 Apr 05
McNeil JS, Calgi MP, Tsang S, Theodore D, Thames MR, Naik BI. Impact of body mass index on surgical case durations in an academic medical center. J Clin Anesth. 2023 Nov;90:111198. PMID: 37441834. Epub 2023 Jul 11
Fox WE, Marshall M, Walters SM, Mangunta VR, Ragosta M, Kleiman AM, McNeil JS. Bedside Clinician’s Guide to Pulmonary Artery Catheters. Crit Care Nurse. 2023 Aug 1;43(4):9-18. PMID: 37524367
Knio ZO, Ising MS, Yount KW, Tanaka K, McNeil JS. Undiagnosed Factor VII Deficiency in Cardiac Surgery Complicated by Bleeding: A Case Report. A A Pract. 2023 Sep 1;17(9):e01713. PMID: 37681735. Epub 2023 Sep 06
McNeil JS. In response. J Clin Anesth. 2023 Dec;91:111266. PMID: 37769408. Epub 2023 Sep 26
Snyder EL, Sekela ME, Welsby IJ, Toyoda Y, Alsammak M, Sodha NR, Beaver TM, Pelletier JPR, Gorham JD, McNeil JS, Sniecinski RM, Pearl RG, Nuttall GA, Sarode R, Reece TB, Kaplan A, Davenport RD, Ipe TS, Benharash P, Lopez-Plaza I, Gammon RR, Sadler P, Pitman JP, Liu K, Bentow S, Corash L, Mufti N, Varrone J, Benjamin RJ, for the ReCePI study group. Evaluation of the efficacy and safety of amustaline/glutathione pathogen-reduced RBCs in complex cardiac surgery: the Red Cell Pathogen Inactivation (ReCePI) study-protocol for a phase 3, randomized, controlled trial. Trials. 2023 Dec 11;24(1):799. PMID: 38082326. Epub 2023 Dec 11
Mazzeffi M, Beller J, Strobel R, Norman A, Wisniewski A, Smith J, Fonner CE, McNeil J, Speir A, Singh R, Tang D, Quader M, Yarboro L, Teman N. Trends in the Use of Recombinant Activated Factor VII and Prothrombin Complex Concentrate in Heart Transplant Patients in Virginia. J Cardiothorac Vasc Anesth. 2024 Mar;38(3):660-666. PMID: 38220518. Epub 2023 Oct 04
Zvara J, Smith AL, Mazzeffi MA, Kleiman AM, Tanaka K, Smith AR, Wilson JM, McNeil JS. Alpha-Gal Syndrome and Cardiac Surgery. J Cardiothorac Vasc Anesth. 2024 Jul 22;S1053-0770(24)00494. PMID: 39097488. Epub 2024 Jul 22
Collins S, Baker EB. Resident Recruitment in a New Era. Int Anesthesiol Clin. 2024 Jul 1;62(3):35-46. PMID: 38855840. Epub 2024 Jun 10
Millan PD, Kleiman AM, Friedman JF, Dunn LK, Gui JL, Bechtel AJ, Collins SR, Huffmyer JL, Dwivedi P, Wolpaw JT, Nemergut EC, Tsang S, Forkin KT. The impact of hindsight bias on the diagnosis of perioperative events by anesthesia providers: A multicenter randomized crossover study. J Clin Anesth. 2024 Jul 12;97:111549. PMID: 39002404. Epub 2024 Jul 12
Mazzeffi M, Miller D, Garneau A, Sheeran J, Kleiman A, Mehta SH, Tiouririne M. Cesarean Delivery Outcomes for Patients with Coronavirus Disease-2019 in the USA. J Racial Ethn Health Disparities. 2023 Nov 8. PMID: 37938434. Epub 2023 Nov 08
Abatzis VT, Park CS, Sumler ML, Littlewood KE. Exploring Fraught Boundaries and Landscapes of Practice. Anesth Analg. 2023 Sep 1;137(3):548-550. PMID: 37590799. Epub 2023 Aug 17
Sumler ML, Abatzis VT, Littlewood KE, Park CS. In Response. Anesth Analg. 2024 Jun 1;138(6):e47-e48. PMID: 38771614. Epub 2024 May 20
Tanaka KA, Mazzeffi MA, Levy JH. Rethinking Coagulation Activation during Extracorporeal Membrane Oxygenation: Insights from the Case of Mr. Hageman. Anesthesiology. 2024 Jul 1;141(1):7-9. PMID: 38860792
Monaco F, Guarracino F, Vendramin I, Lei C, Zhang H, Lomivorotov V, Osinsky R, Efremov S, Gürcü ME, Mazzeffi M, Pasyuga V, Kotani Y, Biondi-Zoccai G, D’Ascenzo F, Romagnoli E, Nigro Neto C, Do Nascimento VTNDS, Ti LK, Lorsomradee S, Farag A, Bukamal N, Brizzi G, Lobreglio R, Belletti A, Arangino C, Paternoster G, Bonizzoni MA, Tucciariello MT, Kroeller D, Di Prima AL, Mantovani LF, Ajello V, Gerli C, Porta S, Ferrod F, Giardina G, Santonocito C, Ranucci M, Lembo R, Pisano A, Morselli F, Nakhnoukh C, Oriani A, Pieri M, Scandroglio AM, Kırali K, Likhvantsev V, Longhini F, Yavorovskiy A, Bellomo R, Landoni G, Zangrillo A. Acute normovolemic hemodilution in cardiac surgery: Rationale and design of a multicenter randomized trial. Contemp Clin Trials. 2024 Aug;143:107605. PMID: 38866095. Epub 2024 Jun 10
Tanaka KA, Stewart KE, Mazzeffi MA. Toward Better Anticoagulation Monitoring for Extracorporeal Membrane Oxygenation: Taking C-reactive Protein Out of the Equation?. J Cardiothorac Vasc Anesth. 2024 Sep;38(9):1897-1898. PMID: 38866660. Epub 2024 Apr 25
Frere C, Mazzeffi M, Maier CL, Helms J, Steiner ME, Sullenger BA, Tanaka KA, Connors JM, Levy JH. Acquired von Willebrand syndrome during extracorporeal membrane oxygenation support: a comprehensive review of current evidence: communication from the ISTH SSC on perioperative and critical care thrombosis and hemostasis. J Thromb Haemost. 2024 Sep;22(9):2608-2628. PMID: 38925492. Epub 2024 Jun 24
Wisniewski A, Norman A, Tsang S, Ricketts R, Sharma R, Suggs J, Vizzini S, Castro B, Raphael J, McNaull P, Gangemi J, Roeser M, Mazzeffi M. Pilot Assessment of Platelet Thrombus Area and Contractile Force in Pediatric Congenital Heart Surgery Patients Using a Microfluidic Device. J Cardiothorac Vasc Anesth. 2024 Sep;38(9):2009-2016. PMID: 38960807. Epub 2024 Jun 17
Williams B, Henderson R, Mazzeffi M, Tanaka K. FEIBA: Too Potent a Potion or Just Right for Post-CPB Bleeding?. J Cardiothorac Vasc Anesth. 2024 Sep;38(9):1882-1884. PMID: 38972817. Epub 2024 Jun 19
Singla P, Brenner B, Tsang S, Elkassabany N, Martin L, Mazzeffi M. Anesthetic technique and postoperative pulmonary complications (PPC) after Video Assisted Thoracic (VATS) lobectomy : A retrospective observational cohort study. PLOS One, 2024
Singla, P., Tsang, S., Mazzeffi, M, Johnson LC, Denton LH, Elkassabany N. Impact of transition of medical journals from print to online-only on their scholarly performance. Scientometrics 129, 2855–2866 (2024). https://doi.org/10.1007/s11192-024-04998-1
Ryan Lee, Samantha Helmy, Jeronimo Cardona, David Zhao, Raymond Rector, Joseph Rabin, Michael Mazzeffi, Sung-min Cho, Nicholas Morris, & Imad Khan. NeuroSurgical Procedures in Patients Requiring ECMO (NSPIRE). Society of Critical Care Medicine 2024 Conference — Abstract Submitted, Manuscript in Process.
Dave SB, Rabinowitz R, Shah A, Tabatabai A, Galvagno SM Jr, Mazzeffi MA, Rector R, Kaczorowski DJ, Scalea TM, Menaker J. COVID-19 outcomes of venovenous extracorporeal membrane oxygenation for acute respiratory failure vs historical cohort of non-COVID-19 viral infections. Perfusion. 2023 Sep;38(6):1165-1173. PMID: 35653427. Epub 2022 Jun 02
Grazioli A, Plazak M, Dahi S, Rabin J, Menne A, Ghoreishi M, Taylor B, Perelman S, Mazzeffi M. Veno-arterial extracorporeal membrane oxygenation without allogeneic blood transfusion: An observational cohort study. Perfusion. 2023 Oct;38(7):1519-1525. PMID: 35957550. Epub 2022 Aug 11
Wargowsky R, Zvara J, Qaddumi N, Gonzalez-Almada A, Lin D, Fernandez X, Tanaka K, Mazzeffi M. In vitro comparison of spatiotemporal fibrin clot formation dynamics in plasma treated with different protamine-heparin ratios. Perfusion. 2023 Nov;38(8):1631-1636. PMID: 36036659. Epub 2022 Aug 29
Raphael J, Feng X, Shotwell MS, Mazzeffi MA, Bollen BA, Shah AS, Kertai MD. Association of Intraoperative Red Blood Cell Transfusions With Venous Thromboembolism and Adverse Outcomes After Cardiac Surgery. Ann Surg. 2023 Sep 1;278(3):e650-e660. PMID: 36538645. Epub 2022 Oct 19
Mazzeffi M, Lin D, Gonzalez-Almada A, Stombaugh DK, Curley J, Mangunta V, Teman N, Yarboro LT, Thiele R. Outcomes of heparinized adult veno-arterial extracorporeal membrane oxygenation patients managed with low and high activated partial thromboplastin time targets: A systematic review and meta-analysis. Perfusion. 2024 Apr;39(3):525-535. PMID: 36595340. Epub 2023 Jan 03
Hensley NB, Colao JA, Zorrilla-Vaca A, Nanavati J, Lawton JS, Raphael J, Mazzeffi MA, Wierschke C, Kostibas MP, Cho BC, Frank SM, Grant MC. Ultrafiltration in cardiac surgery: Results of a systematic review and meta-analysis. Perfusion. 2024 May;39(4):743-751. PMID: 36795704. Epub 2023 Feb 16
Heuts S, Mariani S, van Bussel BCT, Boeken U, Samalavicius R, Bounader K, Hou X, Bunge JJH, Sriranjan K, Wiedemann D, Saeed D, Pozzi M, Loforte A, Salazar L, Meyns B, Mazzeffi MA, Matteucci S, Sponga S, Sorokin V, Russo C, Formica F, Sakiyalak P, Fiore A, Camboni D, Raffa GM, Diaz R, Wang IW, Jung JS, Belohlavek J, Pellegrino V, Bianchi G, Pettinari M, Barbone A, Garcia JP, Shekar K, Whitman G, Lorusso R, PELS-1 Investigators. The Relation Between Obesity and Mortality in Postcardiotomy Venoarterial Membrane Oxygenation. Ann Thorac Surg. 2023 Jul;116(1):147-154. PMID: 37015310. Epub 2023 Apr 02
Shoni M, Lazar S, Jackson A, Tonetti MK, Horak J, Gutsche J, Augoustides JG, Marchant BE, Fernando RJ, Jelly CA, Gallo PD, Mazzeffi MA. Parallel Venovenous Extracorporeal Membrane Oxygenation Circuits for Refractory Hypoxemia in a Super-Super-Obese Patient. J Cardiothorac Vasc Anesth. 2023 Jul;37(7):1304-1314. PMID: 37028990. Epub 2023 Mar 12
Tanaka KA, Butt AL, Abuelkasem E, Mazzeffi MA. Protamine and Coagulopathy After Cardiopulmonary Bypass: May the Perfect Electrostatic Force Be With You. J Cardiothorac Vasc Anesth. 2023 Aug;37(8):1509-1510. PMID: 37120320. Epub 2023 Feb 01
Mazzeffi M, Curley J, Gallo P, Stombaugh DK, Roach J, Lunardi N, Yount K, Thiele R, Glance L, Naik B. Variation in Hospitalization Costs, Charges, and Lengths of Hospital Stay for Coronavirus Disease 2019 Patients Treated With Venovenous Extracorporeal Membrane Oxygenation in the United States: A Cohort Study. J Cardiothorac Vasc Anesth. 2023 Aug;37(8):1449-1455. PMID: 37127521. Epub 2023 Apr 07
Mazzeffi M, Shelton K. Preparing Cardiothoracic Intensive Care Unit Leaders for Success. J Cardiothorac Vasc Anesth. 2023 Aug;37(8):1485-1486. PMID: 37147208. Epub 2023 Apr 14
Flynn BC, Steiner ME, Mazzeffi M. Off-label Use of Recombinant Activated Factor VII for Cardiac Surgical Bleeding. Anesthesiology. 2023 Aug 1;139(2):197-210. PMID: 37155359
Strobel RJ, Money DT, Young AM, Wisniewski AM, Norman AV, Ahmad RM, Kaplan EF, Joseph M, Quader M, Mazzeffi M, Yarboro LT, Teman NR, Investigators for the Virginia Cardiac Services Quality Initiative. Extracorporeal Life Support Organization Center of Excellence recognition is associated with improved failure to rescue after cardiac arrest. J Thorac Cardiovasc Surg. 2024 May;167(5):1866-11877.e1. PMID: 37156364. Epub 2023 May 06
Wieruszewski PM, Coleman PJ, Levine AR, Davison D, Smischney NJ, Kethireddy S, Guo Y, Hecht J, Mazzeffi MA, Chow JH. Trajectory of PaO2/FiO2 Ratio in Shock After Angiotensin II. J Intensive Care Med. 2023 Oct;38(10):939-948. PMID: 37161301. Epub 2023 May 09
Sun GH, Ortoleva JP, Lu SY, Vanneman MW, Tanaka K, Mazzeffi M, Dalia AA. ABO Blood Group and Bleeding and Survival in VA-ECMO Patients. J Intensive Care Med. 2023 Nov;38(11):1015-1022. PMID: 37291851. Epub 2023 Jun 08
Guinn N, Tanaka K, Erdoes G, Kwak J, Henderson R, Mazzeffi M, Fabbro M, Raphael J. The Year in Coagulation and Transfusion: Selected Highlights from 2022. J Cardiothorac Vasc Anesth. 2023 Dec;37(12):2435-2449. PMID: 37690951. Epub 2023 Aug 17
Waterford SD, Holmes SD, Fonner CE, Alejo D, Salenger R, Hensley NB, Mazzeffi M, Ad N, Maryland Cardiac Surgery Quality Initiative. Institutional Variability in Red Blood Cell Transfusion With Coronary Bypass in a Statewide Database. Ann Thorac Surg. 2023 Dec;116(6):1285-1290. PMID: 37739112. Epub 2023 Sep 20
Kertai MD, Makkad B, Bollen BA, Grocott HP, Kachulis B, Boisen ML, Raphael J, Perry TE, Liu H, Grant MC, Gutsche J, Popescu WM, Hensley NB, Mazzeffi MA, Sniecinski RM, Teeter E, Pal N, Ngai JY, Mittnacht A, Augoustides YGT, Ibekwe SO, Martin AK, Rhee AJ, Walden RL, Glas K, Shaw AD, Shore-Lesserson L. Development and Publication of Clinical Practice Parameters, Reviews, and Meta-analyses: A Report From the Society of Cardiovascular Anesthesiologists Presidential Task Force. Anesth Analg. 2024 Apr 1;138(4):878-892. PMID: 37788388. Epub 2024 Oct 03
Kopanczyk R, Lisco SJ, Pearl R, Demiralp G, Naik BI, Mazzeffi MA. Racial and Ethnic Disparities in Veno-Venous Extracorporeal Membrane Oxygenation Mortality for Patients With Severe COVID-19. ASAIO J. 2024 Jan 1;70(1):62-67. PMID: 37815999. Epub 2023 Oct 09
Man L, Yount K, Grazioli A, Padmanabhan A, Thiele R, Maitland HS, Mazzeffi M. Recrudescent Heparin-Induced Thrombocytopenia After Therapeutic Plasma Exchange in a Patient Undergoing Thoracic Aortic Replacement. J Cardiothorac Vasc Anesth. 2023 Dec;37(12):2592-2596. PMID: 37827918. Epub 2023 Sep 21
Raphael J, Chae A, Feng X, Shotwell MS, Mazzeffi MA, Bollen BA, Pfeil D, Feduska E, Shah AS, Kertai MD. Red Blood Cell Transfusion and Pulmonary Complications: The Society of Thoracic Surgeons Adult Cardiac Surgery Database Analysis. Ann Thorac Surg. 2024 Apr;117(4):839-846. PMID: 38216079. Epub 2024 Jan 11
Mazzeffi M, Strickland L, Coffman Z, Miller B, Hilton E, Kohan L, Keneally R, McNaull P, Elkassabany N. Cross sectional study of Twitter (X) use among academic anesthesiology departments in the United States. PLoS One. 2024;19(2):e0298741. PMID: 38330078. Epub 2024 Feb 08
Mazzeffi M, Miller D, Wang A, Kothandaraman V, Money D, Clouse B, Zaaqoq AM, Teman N. Iatrogenic blood loss from phlebotomy during adult extracorporeal membrane oxygenation: A retrospective cohort study. Transfusion. 2024 Mar;64(3):475-482. PMID: 38385665. Epub 2024 Feb 22
Mazzeffi M, Satyapriya SV, Gutsche J. Diverse inputs and complementary skillsets lead to the highest quality patient care in cardiothoracic surgery intensive care units. JTCVS Open. 2024 Feb;17:183. PMID: 38420539. Epub 2023 Dec 07
Panda K, Glance LG, Mazzeffi M, Gu Y, Wood KL, Moitra VK, Wu IY. Perioperative Extracorporeal Cardiopulmonary Resuscitation in Adult Patients: A Review for the Perioperative Physician. Anesthesiology. 2024 May 1;140(5):1026-1042. PMID: 38466188
Glance LG, Joynt Maddox KE, Mazzeffi M, Shippey E, Wood KL, Yoko Furuya E, Stone PW, Shang J, Wu IY, Gosev I, Lustik SJ, Lander HL, Wyrobek JA, Laserna A, Dick AW. Insurance-based Disparities in Outcomes and Extracorporeal Membrane Oxygenation Utilization for Hospitalized COVID-19 Patients. Anesthesiology. 2024 Jul 1;141(1):116-130. PMID: 38526387
Mazzeffi M, Gutsche J. Thermodilution-derived Recirculation and Cardiac Output Measurement during Veno-venous Extracorporeal Membrane Oxygenation: Do We Need More Bells and Whistles?. Anesthesiology. 2024 May 1;140(5):887-889. PMID: 38592358
Keneally RJ, Heinz ER, Jaffe EM, Niak BI, Canonico AB, Roland LM, Chow JH, Mazzeffi MA. Factors associated with unintended perianesthesia hypothermia. Proc (Bayl Univ Med Cent). 2024;37(3):424-430. PMID: 38628320. Epub 2024 Feb 23
Mazzeffi M, Levy JH. Antithrombin Deficiency during Venoarterial Extracorporeal Membrane Oxygenation: Extremely Common, but Does It Matter?. Anesthesiology. 2024 Jun 1;140(6):1065-1067. PMID: 38742999
Mariani S, Ravaux JM, van Bussel BCT, De Piero ME, van Kruijk SMJ, Schaefer AK, Wiedemann D, Saeed D, Pozzi M, Loforte A, Boeken U, Samalavicius R, Bounader K, Hou X, Bunge JJH, Buscher H, Salazar L, Meyns B, Mazzeffi MA, Matteucci S, Sponga S, Sorokin V, Russo C, Formica F, Sakiyalak P, Fiore A, Camboni D, Raffa GM, Diaz R, Wang IW, Jung JS, Belohlavek J, Pellegrino V, Bianchi G, Pettinari M, Barbone A, Garcia JP, Shekar K, Whitman GJR, Lorusso R, PELS Investigators. Features and outcomes of female and male patients requiring postcardiotomy extracorporeal life support. J Thorac Cardiovasc Surg. 2024 May 17;S0022-5223(24)00435. PMID: 38762034. Epub 2024 May 17
Vandyck KB, Mazzeffi MA, Tanaka KA. Sepsis Management: Heeding the Sirens and Navigating Between Scylla and Charybdis. Anesth Analg. 2024 Jun 1;138(6):e44-e45. PMID: 38771612. Epub 2024 May 20
Renwick CM, Curley J. Optic Nerve Ultrasound for Monitoring Deteriorating Intracranial Hemorrhage in a Patient on Extracorporeal Membrane Oxygenation: A Case Report. Cureus. 2023 Jul;15(7):e42719. PMID: 37654933. Epub 2023 Jul 31
Curley JM, Ridley DJ, Kashkooli K, Tsang S. Intraoperative FoCUS: Training Practices and Views on Feasibility. J Cardiothorac Vasc Anesth. 2023 Dec;37(12):2482-2488. PMID: 37690950. Epub 2023 Aug 10
Curley J, Flores-Curley M, Tsang S, Esfahani K. Use of Simulation Resources for Underrepresented in Medicine Youth Engagement: A National Survey of Academic Anesthesiology Programs With Specified Diversity, Equity, and Inclusion Positions. Cureus. 2023 Aug;15(8):e44064. PMID: 37746461. Epub 2023 Aug 24
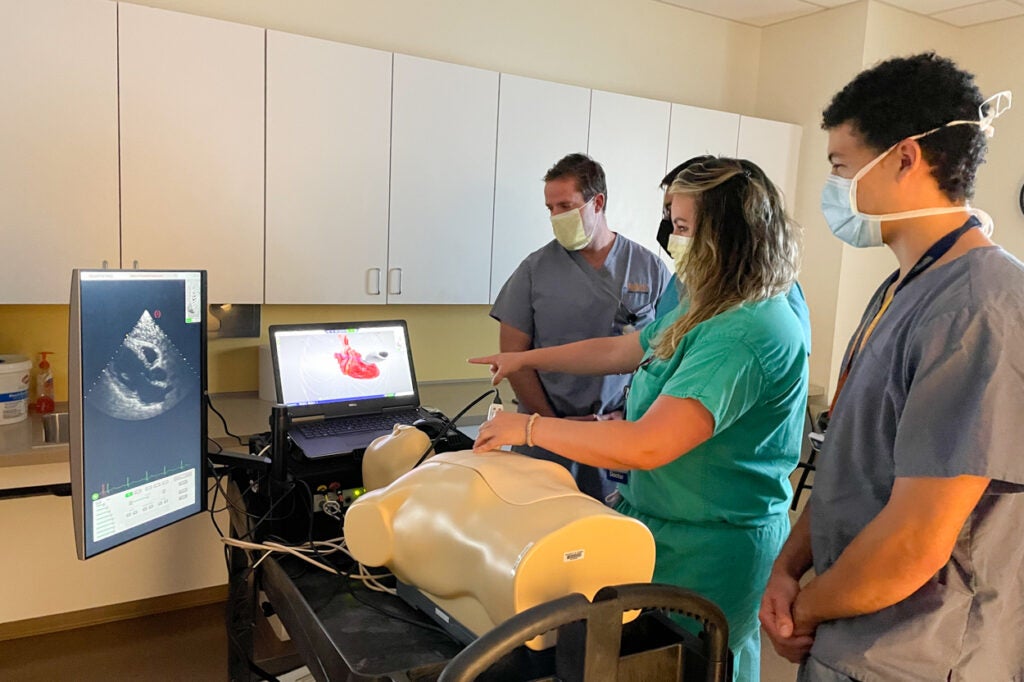
UVA Residents perform cardiac POCUS during a teaching session with the HeartWorks simulator.
Education and Training
Our residents care for the vast majority of cardiac, thoracic, and major vascular cases at UVA. Residents are assigned at least 3.5 months of cardiac, one month of thoracic, and 2 weeks of vascular rotations throughout their residency; in addition, they are often assigned these types of cases on general OR rotations. Prior to their first week on the cardiac rotation, they complete a preparation week involving observation and involvement in cardiac cases, as well as simulation and teaching sessions in the Simulation Center.
A main focus of our division is performing and teaching TEE and focused cardiac ultrasound. Residents rotate through 2-4 weeks of TEE rotation in the operating room where they learn the basics of TEE in cardiac surgery patients, and we frequently incorporate focused transthoracic echocardiography in the perioperative care of noncardiac surgery patients. Additionally, residents train in procedures required for non cardiac thoracic surgery, including regional and neuraxial analgesic techniques, fiberoptic bronchoscopy, advanced airway management techniques, lung isolation and one lung ventilation and lung ultrasound. Outside of the operating room, members of our division are involved in teaching a monthly Perioperative Ultrasound Course lecture or hands-on workshop, and residents are taught point-of-care ultrasound (POCUS) in the simulation center by several faculty in our group during their days set aside for education.