Residency FAQs
Frequently Asked Questions About Our Residency
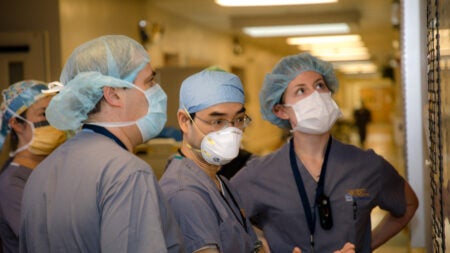
UVA Anesthesia Residents & Attendings check the “Big Board” in the OR for their assignments.
Please reach out at any time to us with additional questions you may have about our program. No questions are off limits!
We want you to find the perfect “HOME” to help you launch your career in anesthesiology! For many of you, we hope that place is UVA Anesthesiology!
Clinical Topics
Our goal is to provide residents with the clinical experience that offers them the greatest educational benefit. Our residents work an average of 60-65 hours per week, depending upon level of training and rotation requirement. While our total hours are slightly lower than the national average, all of our residents achieve case volumes that are considerably above the national averages for cardiac anesthesia, thoracic anesthesia, neuroanesthesia, regional anesthesia, and pediatric anesthesia. We accomplish this by preferentially assigning residents to high quality cases.
In addition to operating room assignments, all residents rotate on the Acute Pain Service and through our nationally regarded Pain Management Clinic for an educational experience that is unparalleled.
We believe that optimal resident education depends upon a balance of didactics, self-directed study, and clinical experience. We coach residents that to be successful in our program and pass the Boards, 5 additional weekly study hours outside of the hospital is a good guide. Some residents come in and study before they set up their rooms, and some do it all in one block on evenings and weekends – this is totally up to what works best for each individual! The resident work schedule follows the ACGME requirements and we adhere strictly to educational and work hour rules.
All of our case volume requirements far exceed the national average and minimum requirements. However, our high-volume rotations are Cardiac and Neuroanesthesia. We also have a busy Pain and Regional service.
The University of Virginia is a tertiary care hospital with a large referral base encompassing the states of Virginia and West Virginia, along with portions of Tennessee, North Carolina, and Maryland. There is also a significant community base for more straightforward cases. Our cases tend to be high quality teaching cases with high acuity, including trauma and organ transplantation.
We are fortunate to have tremendous volumes in all of the clinical areas. Residents rotate through general, ambulatory, cardiothoracic, chronic pain management, ICU, neuroanesthesia, obstetric, pediatric, pediatric cardiac, regional, research, transplant, and trauma.
Our clinical volumes in all areas are well above the national average and far exceed minimum requirements.
Our four-year residents complete month long rotations in the pediatric, surgical, neurologic and cardiac ICUs. Our department has anesthesiologists/intensivists who attend in the surgical, neuro and cardiac ICUs. Most ICUs use a combination of input from anesthesiologists, surgeons, internists, and pediatricians in both semi-open and closed units.
It should be noted that the RRC requires 4 months of critical care, therefore new CA1s without critical care experience in their internship will need to complete 4 months of ICU. Three-year residents who have completed 2 months of ICU in their internship will do 2 months total of cardiac, surgical, or neurologic ICU. Residents interested in pursuing fellowship training in critical care may take additional rotations during their CA3 year.
We are fortunate to have a high volume regional service (>5,000 blocks/year) and pain service (>3,000 blocks/year). Our residents complete rotations in regional anesthesia and in pain management, which includes both acute and chronic pain. These rotations are taught by nationally respected leaders in the area, all of whom have subspecialty training. Training includes ultrasound techniques for upper and lower extremity blocks, continuous catheter techniques, a busy thoracic epidural service, and fluoroscopy guided pain blocks.
Children constitute about 20% of our patient population and our volume of cases (~5,000 cases/year in patients 12 years and under), considerably above the national average. The pediatric experience ranges from procedural sedation to complex craniofacial and cardiac reconstruction. The best part of our experience is that you will be taught by experienced clinician educators. Our 9 pediatric anesthesiologists are board certified in anesthesiology and fellowship trained in pediatric anesthesia.
Most of our residents elect to do additional rotations through OB, cardiac, pediatrics, research, regional, or pain management. The number of months of electives varies with resident interest. Our goal is to train residents for their individual future needs, be it academics, specialties, or private practice. Therefore, we do everything possible to accommodate requests for electives that benefit the resident.
Away rotations are not necessary as all the ACGME requirements for case volume can be met at our hospital. However, several residents each year participate in faculty-led medical missions to South America, Africa, and Asia. Most residents also elect to do an OB rotation at Fairfax Hospital in northern Virginia.
Personal Demographics
In a 2021 survey of 62 residents, 22.6% were single, 35.5 % were married, and 41.9% were in a relationship (non married).
In a 2021 survey of 62 residents, 11.3% of our residents have children and 88.7% don’t have children.
In a 2021 survey of 62 residents, 59.7% have pets while 40.3% don’t have pets.
In a 2021 survey of 62 residents, of the 37 residents who have pets, 51.4% have a dog, 32.4% have a cat and 16.2% have both a dog and a cat.
In a 2021 survey of 62 residents, 80.6% rent and 19.4% own their house.
In a 2021 survey of 62 residents, 51.7% live with roommates/family while 48.3% live alone.
In a 2021 survey of 62 residents, 80.6% drive and 19.4% walk to work.
In a 2021 survey of 62 residents, 62.9% spoke only English while 37.1% spoke another language as well.
Education/Research
There are multiple didactic teaching opportunities available each week at the University of Virginia.
The required, non elective sessions include Monday (CA-0/Ca-1) and Tuesday (CA-2/CA-3) afternoon Resident Conferences and Wednesday morning Grand Rounds Conference. During our Monday/Tuesday afternoon Resident Conference from 4PM-5PM, residents in the operating room are relieved from clinical duties by CRNAs and faculty. The Resident Conference includes case-based discussion, lecture, and journal club formats.
Wednesday Grand Rounds are attended by all residents, CRNAs, and faculty members and are separated into two sessions. The first hour features a resident academic presentation, while the second hour is a faculty academic presentation (both from inside and outside the department as well as by visiting professors). Resident Conference and 8AM Wednesday Grand Rounds sessions follow the topic schedule according to the teaching block curriculum which is repeated every two years.
Designed by our Program Director, one Wednesday per month features our split anesthesia curriculum from 6:30AM-7:50 AM. Basic clinical anesthesia educational topics are covered in a case-based forum for CA0 and CA1 residents. This further prepares CA2 and CA3 residents with a perioperative ultrasound course, including TEE, TTE and critical care ultrasound, in addition to mock oral board case conferences.
Throughout the week there are elective didactic learning opportunities as well. Our chief residents provide a morning report each Thursday at 6AM prior to the start of the operating room schedule. Then on Friday morning at 6AM there is a faculty/resident facilitated morning report. Both of these sessions tend to focus on clinical cases and anesthesia key concepts, suitable for residents throughout their training. In addition, prior to the in-training exam each year, the Department sponsors and organizes a board review course.
Resident education is a departmental priority. We are fortunate to have some of the best teachers in the world in our department. Our Vice Chair for Education, Erin Hennessey, is recognized nationally for innovative teaching in Simulation. Anesthesiology faculty members have won more teaching awards than any other department at the University of Virginia. Three have won the Master Educator award, the School of Medicine’s most prestigious award for GME teaching, the Dean’s Award for Excellence in Teaching, and many others have become members of the University’s Academy of Distinguished Educators.
Residents are taught by nationally recognized teachers in all areas of anesthesia. We are fortunate that many of our faculty members are at the forefront of academic anesthesiology. We have many faculty on the editorial boards of Anesthesiology and Anesthesia & Analgesia and numerous other journals. Our faculty members lecture nationally at the ASA, IARS, ASRA, SEA, and other organizations. UVA faculty have authored and contributed to many major anesthesiology textbooks and monographs and are experts in diverse areas of anesthesiology.
We also have multiple ABA Oral Board Examiners on faculty, and a couple more that recently retired, who still come in and help prepare our residents. Come winter you will find notes on their office doors saying, “Mock Oral Board in Progress, Do NOT Enter!”
The residents evaluate our faculty on their teaching every year. This past year the departmental average score across 11 areas was 3.6/4.0, indicating the amount of dedication and effort the faculty put into teaching and educating the next generation of anesthesiologists.
Nearly 100% of our graduates over the past 30 years have become board certified through the American Board of Anesthesiology (ABA). Every year we have multiple residents honored for scoring in the top 10% of the national cohort on the ABA In-Training Exam (ITE) and the ABA BASIC examination.
Both laboratory and clinical research is available, but not mandatory. Many residents are involved in research leading to publications in peer-reviewed journals and presentations at national meetings. Elective time for research is available upon request and a research track is an option to some residents during the CA3 year. We have NIH-funded laboratories and a host of clinical studies to provide excellent experience in research.
CA2 residents are required to do a Quality Improvement project and present at a Grand Rounds. CA3 residents are required to present a Grand Rounds presentation with a faculty mentor.
Recruitment Process
We are looking for bright, hard-working, inquisitive applicants who will get along with peers and function as a team. Our residents come from all over the country and have multifarious backgrounds and interests. Applicants are screened based on academic achievements and potential.
Once offered an interview, the applicant is offered several dates to join us for an interview. Applicants will have the opportunity to virtually meet with the chair, the Program Director, the Associate Program Director, a Chief Resident, several faculty members, and as many residents as possible. Applicants are ranked based on academics and the personal interviews.
In a 2021 survey of 62 residents, 80.6% are new to the area and 19.4% are from Virginia.
Residents graduate and enter private practice, fellowships, and/or academics. The department has an exceptionally strong record of placing residents in the best fellowship programs for pain, OB, pediatrics, cardiac, ICU, and research. Our former residents practice in 48 different states, creating a network of job opportunities across the country. Additionally, many of our faculty are nationally recognized and can assist in job placement for private practice, fellowships, and academic positions.
Over the last ten years, about half of our graduates enter private practice/academics, while half match into fellowships. Graduate residents match into top fellowship programs across the country, for example Pain Medicine fellowships: University of Virginia, Brigham and Women’s Boston, University of Vermont; Six entered Critical Care fellowships: University of Virginia, Duke, Vanderbilt, University of Washington, University of Iowa, John’s Hopkins; Cardiac Anesthesia Fellowships: Duke, Mayo Clinic, Emory University, UC San Francisco, University of Washington; Pediatric Anesthesia Fellowships: Children’s Hospital Boston, University of Pittsburgh, Cincinnati Children’s, Children’s National Medical Center, D.C., University of Washington, University of Wisconsin, Texas Children’s, Houston; Three entered Regional Fellowships: University of Virginia, Mayo Clinic, Jacksonville, Stanford University; and Research Fellowship at Stanford University. Academic positions were appointed at these institutions: University of Virginia, University of Utah, the Cleveland Clinic, Emory University and the University of Wisconsin.
See more information on recent residency graduates and their placements.
