Kyphoplasty
Balloon Kyphoplasty
 Your doctor has determined that you have a vertebral compression fracture (VCF). This type of fracture can cause severe back pain. Left untreated, one compression fracture can lead to multiple fractures that, in turn, could alter the shape of your spine and adversely affect your overall health.
Your doctor has determined that you have a vertebral compression fracture (VCF). This type of fracture can cause severe back pain. Left untreated, one compression fracture can lead to multiple fractures that, in turn, could alter the shape of your spine and adversely affect your overall health.
Traditional treatment for VCFs is limited to bedrest, bracing and management of pain, often with narcotics. Although appropriate in some cases, this type of treatment does not address the deformity that can occur with multiple fractures.
Balloon Kyphoplasty is a minimally invasive treatment in which orthopaedic balloons are used to gently elevate the bone fragments in an attempt to return them to the correct position. Before the procedure, you will have diagnostic studies, such as x-rays and magnetic resonance imaging (MRI), to determine the exact location of the fracture.
What is a Vertebral Compression Fracture?
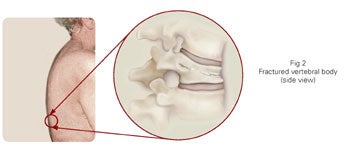
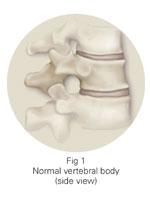 The bones in your spine are called vertebrae; the thick portion of bone at the front of each vertebra is referred to as the vertebral body (Fig 1). A vertebral compression fracture (VCF) occurs when the vertebral body fractures and collapses (Fig 2). Most VCFs are caused by osteoporosis, a disease that causes bones to become brittle and break easily. Because osteoporosis usually progresses without obvious symptoms, a person may not know that they have the disease until a fracture occurs. Compression fractures can also occur as a result of certain types of cancer or tumors.
The bones in your spine are called vertebrae; the thick portion of bone at the front of each vertebra is referred to as the vertebral body (Fig 1). A vertebral compression fracture (VCF) occurs when the vertebral body fractures and collapses (Fig 2). Most VCFs are caused by osteoporosis, a disease that causes bones to become brittle and break easily. Because osteoporosis usually progresses without obvious symptoms, a person may not know that they have the disease until a fracture occurs. Compression fractures can also occur as a result of certain types of cancer or tumors.
 Multiple compression fractures cause your spine to shorten and angle forward, resulting in a stooped posture. This forward curvature of the spine (kyphosis) makes it difficult to walk, reach for things, or conduct activities of daily living.
Multiple compression fractures cause your spine to shorten and angle forward, resulting in a stooped posture. This forward curvature of the spine (kyphosis) makes it difficult to walk, reach for things, or conduct activities of daily living.
Chronic back pain, loss of height, diminished appetite, and difficulty sleeping have been associated with this disorder. Over time, patients with VCFs are at increased risk of suffering from serious, or even fatal, pulmonary complications.
How the Balloon Works
 Balloon Kyphoplasty can be done under local or general anesthesia—your doctor will decide which option is appropriate for you. Typically, the procedure takes less than one hour per fracture treated and may require an overnight hospital stay.
Balloon Kyphoplasty can be done under local or general anesthesia—your doctor will decide which option is appropriate for you. Typically, the procedure takes less than one hour per fracture treated and may require an overnight hospital stay.
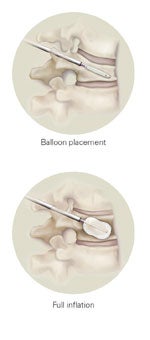
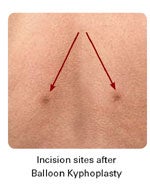
With a hollow instrument, the surgeon creates a small pathway into the fractured bone. A small, orthopaedic balloon is guided through the instrument into the vertebra. The incision site is approximately 1 cm in length.
Next, the balloon is carefully inflated in an attempt to raise the collapsed vertebra and return it to its normal position.
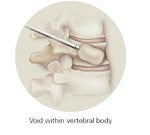
- Once the vertebra is in the correct position, the balloon is deflated and removed. This process creates a void (cavity) within the vertebral body.
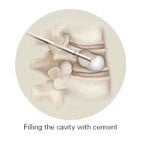
- The cavity is filled with a special cement to support the surrounding bone and prevent further collapse.
- The cement forms an internal cast that holds the vertebra in place. Generally, the procedure is done on both sides of the vertebral body.
After Balloon Kyphoplasty Treatment
Typical postoperative care involves the following:
After the procedure, you will be transferred to the Recovery Room for about an hour. A specially trained nurse will monitor your condition and assess the degree to which your back pain has been alleviated.
During your hospital stay, you will be encouraged to walk and move about. Generally, patients are discharged from the hospital within 24 hours.
Your doctor will have you schedule a follow-up visit and explain limitations, if any, on your physical activity. After treatment with Balloon Kyphoplasty, mobility is often quickly improved. Most patients are very satisfied with the procedure and are able to gradually resume activity once discharged from the hospital.
Frequently Asked Questions
 If a compression fracture is suspected during a physical exam, diagnosis can be easily confirmed with radiographic studies. Compression fractures, however, tend to be under-recognized by physicians and patients alike. The difficulty with diagnosis arises when the discomfort from a compression fracture is mistakenly regarded as simply “back pain” or a “normal” part of aging. Sometimes, a person can have a compression fracture and not have any symptoms at all; this too, can be an obstacle to diagnose.
If a compression fracture is suspected during a physical exam, diagnosis can be easily confirmed with radiographic studies. Compression fractures, however, tend to be under-recognized by physicians and patients alike. The difficulty with diagnosis arises when the discomfort from a compression fracture is mistakenly regarded as simply “back pain” or a “normal” part of aging. Sometimes, a person can have a compression fracture and not have any symptoms at all; this too, can be an obstacle to diagnose.
Over time, the stooped posture and chronic pain associated with multiple compression fractures contribute to an overall poor quality of life. If compression fractures are not diagnosed and consequently, left untreated, the physiological and psychological consequences can be devastating. It is important to have the reason for back pain investigated. Only a complete physical exam, together with an x-ray and MRI, can help your physician determine whether back pain is from a compression fracture or not.
After an initial vertebral fracture, the risk for having another fracture is increased fivefold. In addition, just one VCF affects the distribution of weight along the spinal column. Misalignment brought on by a fractured vertebra places more stress on adjacent vertebrae; the front of the spine has to withstand the same amount of stress with fewer functioning parts, resulting in a structure that is now weakened and vulnerable to additional fracture.
Most VCFs have a gradual onset, unrelated to specific injury or trauma. Fractures can occur as a result of normal activity; i.e., bending over to pick something up, reaching toward something or carrying a bag of groceries. Patients can experience pain ranging from sudden and severe, to persistent and dull. The fact that symptoms of a VCF can be easily confused with other back problems underscores the importance of obtaining a correct diagnosis and receiving treatment.
In cases of multiple fractures, kyphosis can become more pronounced, painful, and debilitating. Forward curvature of the spine has a “compression effect” on your organs, making it progressively difficult to breathe, walk, eat, or sleep properly. Patients with kyphosis have an estimated 24% increase in mortality compared to patients without VCFs.
Studies have shown that patients with multiple compression fractures experience depression, anxiety, and lowered self-esteem, in addition to medical complications. The alteration in lifestyle that accompanies severe kyphosis can profoundly affect a patient’s sense of well-being and cause feelings of isolation and sadness.
In the United States, approximately 150,000 patients are hospitalized every year with compression fractures (average hospital stay 8 days), resulting in costs in excess of $1.6 billion. According to the National Osteoporosis Foundation, the annual direct expenditure (hospitals and nursing homes) for osteoporotic and related fractures has been estimated at $17 billion (2001). This figure translates to $47 million each day, and the cost is rising.
Balloon Kyphoplasty typically takes one hour per fracture treated and may require an overnight hospital stay. The procedure can be done using either local or general anesthesia; the surgeon will determine the most appropriate method, based on the patient’s overall condition.
Balloon Kyphoplasty has been shown to restore vertebral body height and correct spinal deformity with a low complication rate.
Studies also report:
- Significant reduction in back pain
- Significant improvement in quality of life
- Significant reduction in number of days per month that a patient remains in bed; most patients had a 100% reduction in days in bed, one month post-surgery
- Significant improvement in mobility
- Improved ability to perform activities of daily living, such as walking, hobbies, and work
- Significant reduction in number of days where pain interfered with daily activities
Any type of surgery involves risk. Although the complication rate for Balloon Kyphoplasty is low, serious adverse events can occur, including:
- Myocardial infarction (heart attack)
- Cerebrovascular accident (stroke)
- Pulmonary embolism (cement leakage that migrates to the lungs)
- Cardiac arrest (heart stops beating)
Other risks (relevant to the anatomy being treated with bone cement) include deep or superficial wound infection and leakage of cement into the muscle and tissue surrounding the spinal cord. Patients are encouraged to discuss these and other risks, with their physician.
In most cases, Medicare provides coverage for Balloon Kyphoplasty. Other insurance plans may also cover the procedure.
Yes. A physician needs advanced training to perform the procedure. Worldwide, over 4,000 orthopaedic surgeons, neurosurgeons, and interventional radiologists who specialize in treating the spine have already been trained. Physicians who manage osteoporosis (general practitioners, rheumatologists, internists, etc.) can refer patients to a trained spine specialist for treatment. To date, approximately 95,000 fractures in over 75,000 patients have been treated with Balloon Kyphoplasty.
You can get more information on Balloon Kyphoplasty, as well as find a trained spine specialist in your area, by visiting http://www.kyphon.com/.
Need More Information?
Please contact Dr. Jason Sheehan or call our general number (434) 924-2203 (Local) or 1-800-362-2203 (Toll free) and our staff will help you.